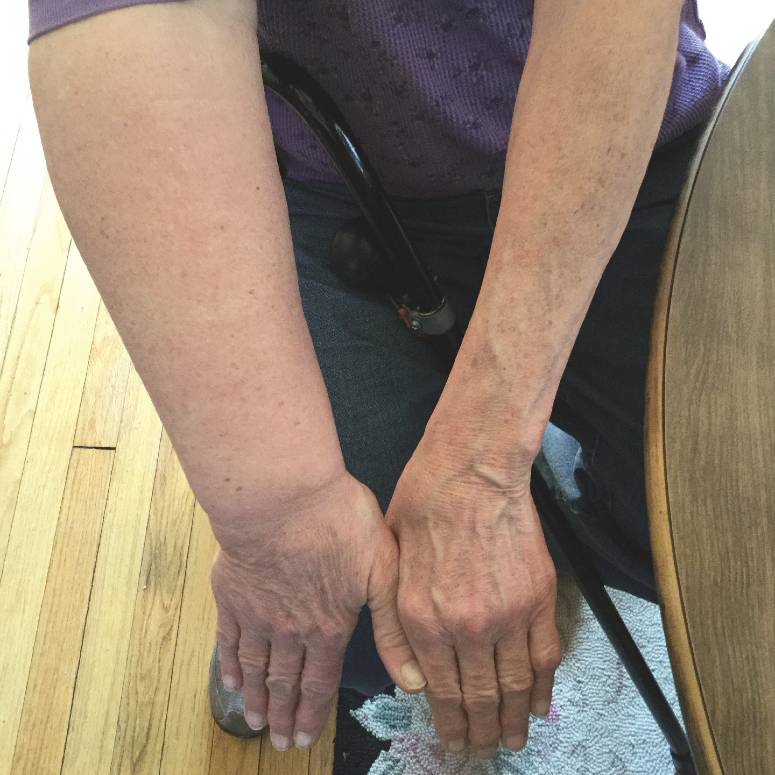
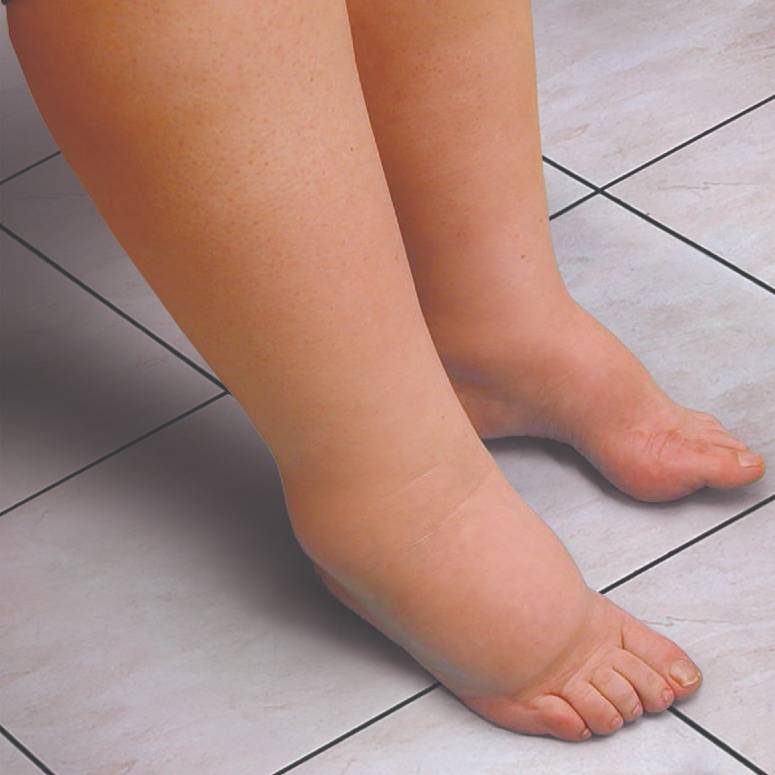
Lymphedema is more common than you think
Lymphedema Causes
Secondary lymphedema is more common. It is the result of known damage or ongoing strain to the lymphatic system, such as:
- Chronic venous insufficiency (CVI)
- Cancer treatments (removal of lymph nodes and/or radiation therapy)
- Benign or malignant tumor growth
- Trauma
Stages of lymphedema
It is important to note that while the following lymphedema stages are commonly recognized, there may be differing levels of severity within each stage.
Stage 0
Swelling may not be apparent despite impaired lymphatic function. Symptoms at this stage may include heaviness, tightness or tingling.
Stage 1
With rest and/or elevation, the swollen limb returns to normal size. Pitting may be present. (When pressure is applied to the skin of the swollen area and released an indentation remains.)
Stage 2
The tissue can present with pitting, but often in this stage more significant skin changes are present with development of fibrosis tissue; the tissue may have a spongy feel.
Stage 3
The tissue at this stage can be hard (fibrotic). The swelling may be largely irreversible and the limb can be very large and swollen. Infections are possible at any stage of lymphedema; however, the risk increases as the stages progress.
Lymphedema Explained
Your lymphatic system is part of your body’s immune system. Its network of tissues, vessels and organs carries lymph fluid, nutrients and waste materials between your body tissues and bloodstream to maintain a normal, healthy fluid balance.
Watch this video to learn more.
Lymphedema Signs and Symptoms
Lymphedema typically appears with the following signs and symptoms:
Limb Heaviness
Limb heaviness is the most common early symptom of lymphedema
Aching, Fatigued Limbs
Aching limbs or unusual and excessive pain/discomfort and fatigue in the limbs
Pitting Edema
Evident when the skin is depressed with your finger for a few seconds and the indentation does not immediately disappear
Swelling (Edema)
Tightness of the skin and awareness that clothing, shoes and jewelry feel tighter in the affected extremity
Decreased Range of Motion
Inability to move your joints and limbs to a normal degree
Decreased Functional Mobility
Inability to stand, walk or move your body normally
Fibrosis
Hardening or scarring of tissue in response to chronic inflammation
Skin Changes
Redness/purplish discoloration, dryness, increased warmth
Decreased Muscle Strength
A feeling of muscle weakness that may lead to physical limitations
Open Wounds
(Venous Ulcers)
A slow-to-heal sore on your leg caused by weak blood circulation in the limb
Stemmer Sign
A thickened skin fold (when pinched at the base of the second toe or finger) that may be a clinical indicator of lymphedema
Pain, Discomfort, Tightness
Lymphedema is often accompanied by a feeling of pain, discomfort and tightness in the affected area
Dysphagia
Difficulty swallowing
Vocal Changes
Including difficulty speaking
Difficulty Breathing
Internal swelling of the larynx can make it difficult to breath
Get Started on a Path To Better Health
Questions? Call us at 1.833.3TACTILE (1-833-382-2845)